Prescription Pain Killer Abuse: From Understanding to Action
Pain is an unpleasant experience that tells you something is wrong. The pain experience happens in the brain and may be a signal to protect part of the body. Acute pain is short-term pain, while chronic pain persists for more than a few months. Chronic pain can be complex and may or may not involve actual tissue damage, emotions, memories and other factors.
Watch Video: “Understanding pain & what to do about it in less than 5 minutes”
Opioids are a class of drugs that alter the chemistry in the brain and body by attaching to opioid receptors. Medically, this class is used as painkillers. These include prescription opioids such as oxycodone, hydrocodone, codeine, morphine, fentanyl and hydromorphone. However, this class also includes illegal drugs like heroin, which is not used medically, but does have a very high abuse potential.
Medically, opioids are used to relieve moderate to severe pain, short-term pain, cancer pain or for anesthesia during surgery. However, opioids are not always indicated for pain and are usually not the best way to treat long-term pain. There is very little science supporting opioid use in long-term non-cancer pain. And side effects and serious risks of these medications, especially when used long-term, are well documented.
Watch Video: “Best Advice for People Taking Opioid Medication”
The Choosing Wisely Initiative provides information to help determine when opioids or alternatives may be considered.
In addition to the serious risks of overdose and addiction, there are additional potential side effects of taking opioid pain medications including developing tolerance to opioids, which means you might need more of the medication for the same pain relief, developing physical dependence on opioids, which means that you have symptoms of withdrawal, like drug craving, anxiety, insomnia, abdominal pain, vomiting, diarrhea, and tremors, if the medication is abruptly stopped.
Chronic opioid use may also cause narcotic bowel syndrome, where the medications may actually cause pain, constipation, bloating and nausea.
Other side effects include constipation, nausea, vomiting, dry mouth, sleepiness, dizziness, confusion, and increased sensitivity to pain.
Some people who start taking opioid pain medications eventually have serious problems with them and become addicted. The opioid epidemic refers to a dramatic increase in the amount of opioids prescribed and the continued increase in drug overdose deaths in the United States. Use of prescription pain medication has nearly quadrupled from 1999 to 2015. In that same time period, opioid overdose deaths have also quadrupled. More Americans die from drug overdoses than in motor vehicle accidents.
Now that the DEA and other agencies have started cracking down on unrestricted prescribing, some people are turning to heroin, which has become cheaper and more available, to support their addiction. Increased opioid use and the lack of supporting science along with more adverse drug events like overdose and death is now being called the opioid epidemic.
First we must understand that drug addiction is a complex chronic brain disease characterized by drug craving, seeking and use despite the negative consequences. Opioid addiction refers to craving, seeking and use of opioids despite negative consequences such as relationship problems, financial problems, functional decline and loss of a job. Opioid addiction can change how the brain works and change how the person thinks, acts and feels.
There is hope for people who have become addicted to prescription opioids or heroin to lead normal lives again. The American Society of Addiction Medicine (ASAM) has been spreading the news with a simple message: “Treat Addiction – Save Lives.”
Opioid abuse refers to taking opioids in a manner that is not prescribed. This includes taking illegal opioids, taking opioids prescribed to another person, taking more than prescribed doses or mixing opioids with other substances. Both illegal and prescription opioids can be abused.
Most often, prescription opioids of abuse are obtained from a friend or relative. Most people don’t know that sharing prescribed opioids is a felony.
People who become addicted to opioids are not able to quit or cut back on them. They often experience issues in their lives linked to opioid use. Signs of addiction include:
- Using more of the opioid than intended or prescribed.
- Attempts to cut back or quit, usually many times and with little success.
- Significant “down time” when you are not very functional due to either intoxication or withdrawal.
- Cravings for opioids when you don’t have them.
- Failure to fulfill important roles and responsibilities in life because of opioids.
- Problems with relationships with family, friends, or co-workers related to opioid use.
- Decreased social or recreational activities, preferring to use or seek after drugs instead.
- Hazardous use, such as driving when you probably shouldn’t be behind the wheel.
- Continued use in spite of known physical or mental health problems caused by the opioids.
- Tolerance, where higher doses are required to get the same effect.
- Withdrawal symptoms when the drug is stopped abruptly.
If you meet at least 4 of these 11 criteria, you have at least a moderate addiction, and if you meet 6 or more you have a severe addiction problem.
Physical dependence is when your body gets used to having a substance on board and without it you will have symptoms of withdrawal. People who take opioids on a daily basis for long enough will become physically dependent. This is not the same thing as addiction.
Opioid withdrawal refers to the symptoms that happen when opioids are stopped. Although symptoms such as headache, nausea, vomiting, diarrhea, cramping, sweating, and flu-like symptoms can be severe and uncomfortable, withdrawal is rarely life-threatening. These withdrawal symptoms typically last for several days. However, depression or mood changes may last for several weeks or even months.
Withdrawal symptoms may be minimized with some medications to treat nausea, aches, cramps or diarrhea. Slowly decreasing opioid dosing may also help minimize withdrawal symptoms.
Opioids may cause death by effecting the part of the brain that regulates breathing. This may cause respiratory depression (slow, shallow or no breathing) and death.
Accidental overdose can happen if a person takes too much pain medication, mixes pain medication with other substances (medications, drugs, or alcohol) or has an adverse drug reaction to prescribed doses of pain medication.
There is an opioid reversal agent called naloxone (also known as NARCAN).
It is important to understand the risks of opioids which include:
- Central nervous system and respiratory depression
- Sedation, memory problems or difficulty thinking
- Risk of falls and fractures
- Worsening pain syndromes, referred to as opioid induced hyperalgesia
- Motor vehicle accidents
- Sexual side effects (hypogonadism)
- GI side effects such as nausea, constipation, dry mouth
- Narcotic bowel syndrome
- Reduced overall quality of life
Abstinence-based treatment programs may not be effective and may be dangerous. When a person goes through a period of time not taking opioids, their tolerance for opioids decreases. If they relapse or begin using opioids again, risk of overdose is high. Studies have shown that the months after leaving an abstinence-based treatment program have a much higher risk of overdose than if the patient received no treatment at all.
Medication-assisted treatment (MAT) includes medication to treat opioid use disorder. MAT increases success of OUD treatment and decreases risk of overdose.
In order to achieve and maintain sobriety off of opioids, most patients will need medication in addition to counseling. All patients with serious opioid use disorders should be considered for MAT.
12 step programs such as Alcoholics Anonymous and Narcotics Anonymous (as well as other self-help groups such as Celebrate Recovery and Rational Recovery) can be helpful to many people with addictions. These programs are not the same as treatment – their focus is to help people stay in recovery. Patients who are on medication for addiction should stay on the medication – even though some 12 step groups discourage medications, it is important to find groups that support the best treatment practices.
12 step programs are not for everyone – they are highly effective for some people but they are not a “one size fits all” solution. Each person suffering from addiction is unique and should have a treatment plan tailored to his or her specific needs. Addiction is a difficult condition to treat, and patients should take advantage of as many aspects of their recovery program as they can, including counseling, medication, spiritual and family involvement, work place recovery, and 12 step groups as appropriate.
Opioid Overdose Rescue and Response: Naloxone
Remember: An overdose is a medical emergency – call 911 immediately
Naloxone is a medication used to REVERSE the effects of opioids, including overdose. Naloxone is an opioid antagonist, which means it binds to the opioid receptor and blocks the opioid. This reverses the effects of the opioid on that receptor. When this blocks or reverses the opioid, breathing is restored. This also may cause abrupt opioid withdrawal.
No. Naloxone cannot be used to get high.
Naloxone is supplied as a single dose nasal inhaler, a single dose auto-injector or in a kit that may require some items be put together before use. Be familiar with the option available to you.

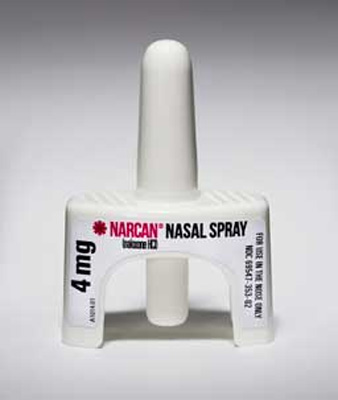
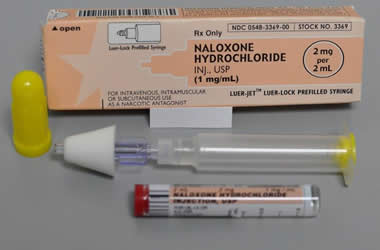
Naloxone should be used when an overdose is identified or suspected.
Signs of an overdose:
- No response when you yell the person’s name or rub the middle of their chest with your knuckles.
- Slow breathing or no breathing (less than 1 breath every 5 seconds)
- Pale or clammy face
- Blue or gray lips, fingernails or skin
- Slow, erratic or no pulse
- Choking or gurgling noises
Recognizing an overdose:
- Check for unresponsiveness, shaking won’t wake the person
- Listen for snoring or choking, slow breathing or no breathing
- Look for blue or gray lips or fingernails
- Touch sweaty or clammy skin
If the person is unresponsive or showing signs of overdose:
Give Naloxone
- Nasal spray: the entire dose is dispensed into one nostril
https://www.narcan.com/ - Auto-injector: follow voice prompts from device to deliver injected dose
https://evzio.com/patient/about-evzio/index.php - Naloxone Nasal Spray Kit for Assembly:
http://dphhs.mt.gov/Portals/85/publichealth/documents/EMSTS/Opioids/Opiod%20Brochure%202017.pdf
Then What?
- Call 911! Activate emergency medical services (EMS). EMS should always be contacted if an opioid overdose is suspected. If EMS has not been called before naloxone is administered, call directly after use.
- Begin CPR if the person is unresponsive and not breathing.
- Consider second naloxone dose. If the person does not respond by waking up in 2-3 minutes, administer another dose of naloxone. Continue CPR.
- If the person is breathing but unresponsive, place the person on their side in the recovery position and watch them closely until EMS arrives.
- If the person does respond, keep them calm, and be ready to give the second dose if the person becomes unresponsive again.
Naloxone is safe regardless of opioid use status. Naloxone will have no effect on a person that does not have opioids in their body.
Naloxone may cause withdrawal symptoms including headache, nausea, vomiting, diarrhea, tremor, sweating, and changes to heart rate and blood pressure. Withdrawal symptoms can be uncomfortable but are not life-threatening.
Remember:
- Naloxone is safe regardless of opioid use status. If the person does not have an opioid in their body, naloxone will not have an action.
- Naloxone is safe in pregnancy.
- Naloxone should be used if an overdose is suspected and the person is not responsive or breathing slowly, irregularly or not at all.
- Naloxone will cause withdrawal – expect it.
Nasal inhaler: https://www.youtube.com/watch?v=hGVSaO1oxpg
Auto-injector: https://www.youtube.com/watch?v=-DQBCnrAPBY
Naloxone nasal kit: https://www.youtube.com/watch?v=WoSfEf2B-Ds
Naloxone injection kit: https://www.youtube.com/watch?v=lg1LEw-PeTE
Additional patient education videos: http://prescribetoprevent.org/patient-education/videos/
Naloxone is available by prescription from your doctor/provider.
Naloxone is also available from participating pharmacies by standing order. This means that the pharmacist may dispense naloxone without a prescription from your doctor/provider.
The Montana DPHHS Opioid Overdose Recognition and Response Guide can be found here: https://dphhs.mt.gov/assets/publichealth/EMSTS/opioids/Naloxonebrochure.pdf
Information for the public as well as prescribers can be found on the Naloxone (mt.gov). The webpage provides an overview of the opioid crisis in Montana along with the standing order, education about overdose recognition and response, and the CDC guidelines for prescribing opioids.
Check with your local pharmacy to see if they are participating in the Standing Order for Naloxone Program.
How to Get Help
If you are in need of immediate help, or experiencing thoughts of suicide, call 9-1-1. Prevention and early intervention is very important and can potentially prevent addiction or diversion problems from becoming irreversible.
There are many considerations for treatment. However, it starts with recognizing a need and then seeking professional assistance. You should always seek professional treatment – detox from prescription painkillers can be dangerous and may require medical treatment throughout the process.
The National Institute on Drug Abuse offers treatment resources for patients and families and a publication called Seeking Drug Abuse Treatment: Know What to Ask, that can assist individuals in finding the right kind of treatment for them.
Montana Pain Management Clinics:
- St. James Healthcare, Butte, MT
- Bozeman Health Pain Management Services, Bozeman, MT
- St. Peter’s Health Pain Management Clinic, Helena, MT
- Benefis Pain Management Center, Great Falls, MT
- Great Falls Clinic, Craig Sweeney, Great Falls, MT (Osteoarthritis & Chronic Pain Letter)
- The Montana Center for Wellness and Pain Management, Kalispell, MT
- Montana Spine and Pain Center, Missoula, MT
Montana Drug/Alcohol Treatment Centers:
- Rimrock Foundation Addiction Treatment Center, Billings, MT
- Acadia Montana, Butte, MT
- Alcohol and Drug Services of Gallatin Valley, Bozeman, MT
- Gateway Recovery Center, Great Falls, MT
- Rocky Mountain Treatment Center, Great Falls, MT
- Community Medical Services, Missoula, MT
- Western Montana Mental Health Center, Missoula, MT
- Wrapped in Hope – St. Luke Community Healthcare, Ronan, MT
- Recovery Center, Missoula, MT
- Helena Indian Alliance, Helena, MT
- Northern Winds Recovery Center, Browning, MT
- Reiter Foundation, Anaconda, MT
Medication-assisted treatment (MAT) is a strategy that uses both medications and behavioral therapies to treat substance use disorders. This combination approach is effective for treatment of and recovery from substance use disorders. These medications curb cravings and may block the effects of opioids. This helps people manage their disease, enter recovery and avoid relapse.
Strong scientific studies show that for opioid addiction, medication is overwhelmingly the essential component of treatment. Treatment of opioid use disorder without medication-assisted treatment may be dangerous and may increase the risk of death from overdose. Several guidelines have been published recommending the use of medications in the treatment of opioid addiction for almost all patients.
Medication Assisted Treatment (MAT) is by far the most effective treatment and should be considered for every person who needs treatment for opioid addiction.
The most common medications used to treat opioid addiction are buprenorphine, methadone and naltrexone. Each medications works differently and each has risks and benefits. Medication therapy is individualized based on patient needs, goals and response
Watch Video: “Treatment Can Help Curb the Opioid Epidemic”
SAMHSA provides a Treatment Service Locator
ASAM Pocket Card “Opioid Addiction Treatment Guide for Patients, Families and Friends”
- The Montana Department of Public Health & Human Services offers many resources on behavioral health services, laws and other related information.
- Montana’s Addictive and Mental Disorders Division or (888) 866-0328.
- The Substance Abuse and Mental Health Services Administration provides several links and help hotlines. This includes easily finding alcohol and drug abuse treatment or mental health treatment facilities and programs around the country.
- National Suicide Prevention Lifeline or 1-800-273-TALK (free, confidential, 24/7)
- Narcotics Anonymous
- National Council on Alcoholism and Drug Dependence
- Rocky Mountain Poison Center for emergencies: 1-800-222-1222
- State Approved Chemical Dependency Treatment Programs
- SAMHSA’s Behavorial Health Treatment Services Locator or call National Helpline 1-800-662-HELP (4357)
Storage & Disposal
Join Operation Medicine Cabinet Montana in your area.
Montana DPHHS maintains a map of locations where you can dispose of all prescription drugs safely. The map can be found below so you can find your nearest location
How To Properly Store Prescription Drugs
70% of prescription drug abusers over the age of 12 report that they are able to get prescription drugs from family and friends. Safe and secure storage is important in helping to prevent prescription drug abuse and diversion.
Safe: Store medication in a cool, dry area
Secure: Secure all medications away from children and pets. Consider locking up all controlled substances to prevent theft and accidental poisoning.
Expiration: Check all expiration dates. Properly dispose of expired meds.
The National Council on Patient Information and Education has information on properly storing your medications.
How To Properly Dispose of Prescription Drugs
Protect children, pets, family members, our community and our environment.
Montanans can properly dispose of unwanted or unused prescription drugs in the following ways.
- Drop unwanted drugs at a permanent prescription drop location or participate in a drug take-back in your community. Prescription drop locations across the state are available by clicking here.
- Follow the disposal steps recommended by the Office of the National Drug Control Policy.
- Take your prescription drugs out of their original containers.
- Mix drugs with an undesirable substance, such as cat litter or used coffee grounds.
- Put the mixture into a disposable container with a lid, such as an empty margarine tub, or into a sealable bag.
- Conceal or remove any personal information, including the prescription number, on the empty containers by covering it with black permanent marker or duct tape, or by scratching it off.
- Place the sealed container with the mixture and the empty drug containers in the trash.
Disposal Locations
Big Timber: 201 W. 1st. Ave. – Sweet Grass County Sheriff’s Office – 932-5143
Billings: 220 North 27th St. – Billings PD – 657-8460
Billings: 2300 Lake Elmo Drive – MT Fish and Game Office – 247-2940
Billings: 2915 Gabel Road – Military Reserve Center – 324-5404
Billings: 2910 3rd Avenue N – Crime Prevention Center – 247-8590
Billings: 4848 Midland Road – Solid Waste Division – 247-8633
Bozeman: 30 North Rouse Avenue – Bozeman Police Department – 582-2234
Bozeman: 615 South 16th St. – Bozeman PD/ Gallatin County Sheriff’s Office – 582-2100
Butte: 225 Alaska St. – Butte-Silver Bow Law Enforcement Dept. – 497-1125
Chinook: Blaine County Sheriff’s Dept. – Blaine County Sheriff’s Dept. – 357-3260
Columbia Falls: 130 6th. St., West – Columbia Falls Police Department – 892-3234
Dillon: 2 S. Pacific Dr., #16 – Beaverhead County Sheriff’s Office – 638-3700
Eureka: 855 Highway 93 North – North Lincoln County Law Enforcement Center – 297-2121
Glasgow: 501 Court Square – Valley County Sheriff’s Office – 228-4333
Great Falls: Montana Highway Patrol – 812 14th St. N. – MHP District II – 453-1121
Hamilton: 223 S. 2nd. St. (City Hall) – Hamilton PD – 363-2100
Havre: 520 4th – Havre PD – 265-4361
Helena: 221 Breckenridge – Helena PD – 457-8830
Kalispell: 920 South Main – Flathead County Sheriff’s Office – 758-5585
Laurel: 215 West 1st Street. – Laurel Police Department. – 628-8737
Libby: 512 California Ave – Lincoln County Sheriff’s Office – 293-4112
Livingston: 414 E. Callender – Park County Sheriff’s Office – 222-4101
Malta: 314 S. 2nd Ave. West – Phillips County Sheriff’s Office – 654-2350
Missoula: 435 Ryman – Missoula PD – 552-6316
Stevensville: 206 Buck Street – Stevensville Police Department – 777-3011
Superior: 310 River St. – Mineral County Sheriff’s Office – 822-3555
Townsend: 519 Broadway – Broadwater County Sheriff’s Office – 266-3441
Troy: 301 E. Kootenai Avenue – Troy Area Dispatch – 295-4111
White Sulphur Springs: 101 W. Crawford – Meagher County Sheriff’s Office – 547-3397
Whitefish: 275 Flathead Ave. – Whitefish Police Department – 863-2420
Patient FAQs
For information on commonly abused drugs, see Commonly Abused Drugs, for a chart containing information on street and commercial names of abused drugs and their health consequences.
- Illicit drug abuse: $181B
- Alcohol abuse: $235B
- Tobacco: $193B
Beyond the raw numbers are other costs to society, including:
- the spread of infectious diseases such as HIV/AIDS and hepatitis C either through sharing of drug paraphernalia or unprotected sex;
- deaths due to overdose or other complications from drug use;
- effects on unborn children of pregnant drug users; and
- other effects such as crime, unemployment, domestic abuse, family dissolution, and homelessness.
- NIDAMED Resources for Medical and Health Professionals
- NIDA Notes (Research News and Trends)
- Research Reports on Different Drugs of Abuse and Related Topics
- NIDA DrugFacts for Science-Based Facts on Drug Abuse and Addiction
- NIDA Addiction Science & Clinical Practice, NIDA’s Peer-Reviewed Journal
For teachers and students, NIDA Goes Back to School provides science-based drug abuse education materials geared to students in grades K-12 and their teachers. All of these materials are free. Students are encouraged to join Sara Bellum, a budding neuroscientist, as she explores the effects of various drugs on the brain. Students and teachers can learn through the Mind Over Matter curriculum, or they can go online to join in Sara’s Quest an interactive web-based program. Educationally appropriate materials from NIDA’s collaboration with Scholastic Marketing Partners, the in-school marketing division of Scholastic, the global children’s publishing and media company, also are available in compilations by year from NIDA’s publications catalog and online through NIDA Goes Back to School. These products include articles and posters from the Heads Up: Real News About Drugs and Your Body program through which Scholastic features NIDA science-based articles on drug abuse and addiction in its Classroom Magazines. ScholasticNews.com also maintains a Heads Up Web site at headsup.scholastic.com. Also available is Marijuana: Facts for Teens and a companion booklet, Marijuana: Facts Parents Need to Know.
YES! The good news is there are alternatives to opioids.
Acetaminophen
Non-steroidal anti-inflammatory drugs (NSAIDs)
Antidepressants
Anticonvulsants
Muscle relaxants
Topical therapies
Acupuncture
Behavioral therapies
Biofeedback
Chiropractic
Diet and nutritional counseling
Exercise
Health coaching
Massage
Pain group
Stretching
Weight management
Yoga, tai chi
Taking Prescription Opioids
Risks of taking opioids include: respiratory depression and death, overdose, sedation, confusion, memory problems, motor vehicle accidents, falls, worsening pain, addiction, and reduced quality of life. Other side effects may include nausea, vomiting, constipation, itching, urinary retention and dry mouth.
- Do take only as prescribed and ask questions
- Do tell your doctor about all other medications you take
- Do read instruction sheets included with your prescriptions
- Do keep all medications secure
- Do dispose of all leftover medications properly
- Do know signs and symptoms of an overdose
- Do know how to use naloxone rescue medication
- Do get HELP 1-800-662-HELP (4357) if you or someone you know is struggling with addition
- Don’t take more medication than prescribed
- Don’t mix medications with alcohol or other drugs
- Don’t share your medications – sharing controlled substances is a felony
- Don’t ever take medications not prescribed to you
- Don’t dissolve crush, cut or chew medications unless instructed to do so
If your doctor prescribes an opioid pain medication, be sure to ask these simple questions.
- Is my pain medication an opioid?
- When should I take this medication?
- How long should I take this medication?
- What level of pain relief is considered effective?
- Do I need to take every pill?
- How can I stop taking this medication?
- Are there non-opioid alternatives that I could choose?
- What if I have a history of tobacco, alcohol or drug addiction?
- Could this medication interact with my sleeping or anxiety medication or OTC?
- What else should I be doing to manage my pain?
- Is naloxone rescue medication right for me?
Useful Links
- Montana Department of Health & Human Services
- U.S. Food and Drug Administration
- United States Department of Justice
- NIDA for Teens
- DEA
- Storage & Disposal
- Centers for Disease Control & Prevention
- Montana DPHHS Mental Health Resources
- US Department of Health and Human Services
- NIH
- National Safety Council – Prescription Pain Killers
- Partnership for Drug-Free Kids
- VHA Pain Management
